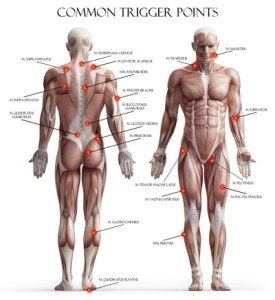
Dry needling helps with managing musculoskeletal pain, functional movement and postural complaints. Myofascial pain is probably the most common condition physiotherapists see worldwide. It affects ups to 10% of the adult population and can account for acute and chronic pain complaints. Commonly myofascial pain results in trigger points, which are typically recognized by palpable nodules in taut bands of tissue. The perpetuating factors of myofascial pain syndromes are low-level musculature contraction, unaccustomed eccentric contraction, muscle overloads, and muscle fatigue.
These factors can be caused by, but not limited to:
- mechanical dysfunctions such as forward head postures
- joint hypermobility
- ergonomic stressors
- poor body mechanics
- Scoliosis.
What is Myofascial?
As far back as the 16th century, myofascial pain syndromes have been recognised as causing sensory, motor and autonomic symptoms and dysfunctions. However, it wasn’t until the 1900’s that it was discovered that the origin of myofascial pain was the trigger points and that the stimulation of the trigger point referred pain. Initially, injection of an analgesic medication into the trigger points produced a decrease in a patient’s symptoms, pain, and the sensitivity to touch of the trigger points. Further research discovered that the actual insertion and stimulation of the muscle with a dry needle produced pain relief without the need for medication. Thus, the development of trigger point dry needling began.
Myofascial trigger point dry needling has no similarities with traditional acupuncture except for the tool being used during the process. Traditionally, acupuncture is based upon Chinese medicine that seeks to regulate flow and stability of energy through subcutaneous placements of needles. Acupuncture points are points mainly along the paths of energy flow (or meridians). In contrast, trigger point dry needles are inserted into specific musculature, targeting tight muscles, and based on neuromuscular and biomechanical principles.
The Dry Needling technique
Studies have found that inserting a dry needle into a trigger point is a very effective way to release trigger points. The theory behind the dry needling technique comes from Dr Chan Gunn, who contributed to the development of dry needling and introduced the term intramuscular stimulation (IMS), in which he described that myofascial pain syndromes are a result of radiculopathy or peripheral neuropathy, causing a disordered function of the peripheral nerve.
This concept is referred to as the radiculopathy model and is based on the Cannon and Rosenblueth’s law of denervation, which states that free flow of nerve impulses maintains innervated function and integrity of structures. When any neural flow is disrupted, all the structures that are innervated by that nerve, such as skeletal muscle, smooth muscle, spinal neurons, sympathetic ganglia, and sweat glands, are affected and can become atrophic, highly irritable, and hypersensitive. The trigger point model describes myofascial trigger points consisting of taut musculature bands due to the excessive release of acetylcholine. Myofascial trigger points are classified as active or latent.
Active myofascial trigger points can cause local and referred pain, or other parasthesias, whereas latent myofascial trigger points may not produce pain without being stimulated. Active myofascial trigger points typically refer pain to a particular site, and these sites are not restricted to a single segmental or peripheral nerve distribution. Clinically, myofascial trigger points can cause motor dysfunction or muscle weakness as a result of motor inhibition, restricted motion, and muscular stiffness. Furthermore, sensory dysfunctions may be noted through localized tenderness, referral of pain to specific areas, hyperalgesia, and/or allodynia.
What treatment can you get from dry needling?
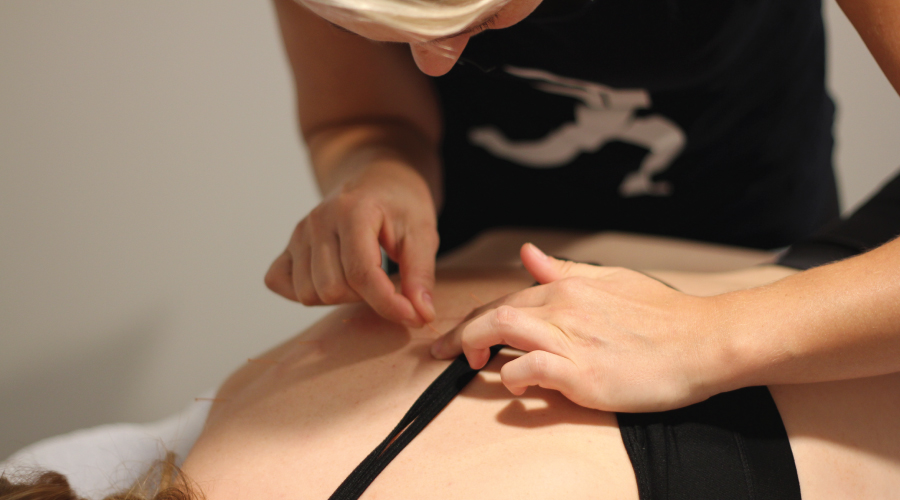
The goal of dry needling is to produce a twitch response (short contraction) of the muscle being needled. The twitch of the muscle is the desired response; however, benefits can occur even without a twitch of the muscle. The simple insertion of the needle into the taut bands can interrupt the pathogenic process and produce mechanical changes in the tissue. The insertion of a needle into the trigger point can produce a deep ache or cramping pressure that lasts only briefly. Reproduction of pain and referral of symptoms may also occur, and soreness may last up to 24–48 hours. Improvements in functional range of motion, decrease in complaints of pain, and ease of mobility may be seen after treatment.
Trigger point dry needling is a relatively new technique in physiotherapy. Internationally, Australia, Belgium, Canada, Chile, Denmark, Ireland, The Netherlands, New Zealand, Norway, South Africa, Spain, Sweden, and Switzerland have recognized trigger point dry needling to be within the scope of practice for a physical therapist.
Clinically, The Body Refinery physiotherapists have found dry needling to be very effective in managing pain in both acute and chronic patients. Our Physiotherapists have also found dry needling to be highly effective in clients with movement and postural complaints. It is a quick easy way to release muscle trigger points prior to therapeutic exercises and the release is maintained well by exercise.
_ _ _
Book an appointment with a Physiotherapist today on 07 3358 3915 or at info@thebodyrefinery.com.au
Follow us on Facebook, Instagram and Twitter for a daily dose of Pilates and Wellbeing.