Bone health is something many people don’t think about until later in life, yet our bones are living structures that respond to how we move, fuel, and care for our bodies. After our mid-30s, bone density naturally begins to decline, and for women, the onset of menopause can accelerate these changes significantly. The good news is that bone loss is not inevitable – with the right exercise, nutrition, and lifestyle strategies, it is possible to maintain strong, healthy bones at any age.
At The Body Refinery, we are passionate about empowering people to take an active role in their musculoskeletal health. Whether you want to prevent bone loss, improve your strength, or manage osteoporosis safely, understanding the factors that influence bone health is the first step.
What Happens to Our Bones as We Age?
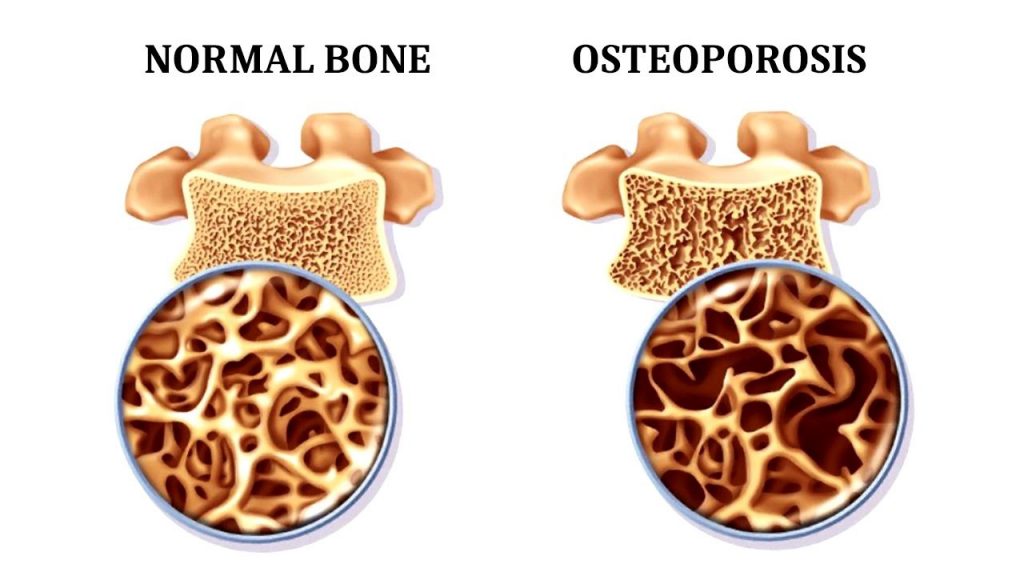
Bone is a dynamic tissue. Throughout life, old bone is continuously broken down and replaced with new bone – a process known as bone remodelling. We reach peak bone mass in our late 20s to early 30s, after which the balance gradually shifts toward more bone being lost than built.
For women, hormonal changes during menopause play a major role. Oestrogen is protective of bone tissue, and its decline can lead to a rapid drop in bone density over the first five to ten years following menopause. This increases the risk of conditions such as osteopenia and osteoporosis, as well as fractures.
However, ageing is not the only factor that influences bone strength. Nutrition, physical activity, genetics, medications, and overall health all contribute to the quality and resilience of your bones.
Key Factors That Influence Bone Health
- Physical Activity
Weight-bearing exercise and resistance training create the mechanical stress that bones need to stay strong. Activities that challenge muscles – such as Pilates, gym-based strength training, and functional movement – stimulate bone formation and improve balance, posture, and coordination, reducing the risk of falls.
- Nutrition
Calcium and vitamin D are essential for bone health. Protein intake also plays an important role in maintaining bone and muscle mass. A well-balanced diet that includes dairy or fortified alternatives, leafy greens, nuts, seeds, and adequate sun exposure (or supplementation when needed) supports bone strength.
- Hormonal Changes
Menopause significantly impacts bone density due to declining oestrogen levels. Individuals who experience early menopause or prolonged amenorrhoea may be at greater risk and benefit from early assessment and intervention.
- Lifestyle Factors
Smoking, excessive alcohol, chronic stress, and low physical activity levels can negatively affect bone health. Building positive lifestyle habits helps protect bone quality throughout life.
How Exercise Supports Strong, Healthy Bones
Research consistently shows that exercise is one of the most effective ways to maintain or improve bone density. The most beneficial types include:
Weight-Bearing Exercise
Activities that require your body to work against gravity — such as walking, stair climbing, low-level impact training, or dynamic functional movement — encourage healthy bone turnover.
Resistance Training
Progressive strength training helps stimulate bone formation by increasing muscle pull on the bone. Heavier, supervised resistance work has been shown to improve bone density in the spine and hips, two common fracture sites.
Balance and Strength for Fall Prevention
Improving strength, stability, and coordination is essential in reducing the risk of falls, which are the leading cause of fractures in older adults.
Pilates, especially when performed with specialised equipment such as the reformer or trapeze table, provides resistance-based loading and can be adapted to safely support those with low bone density.
How The Body Refinery Can Help
The Body Refinery offers a multidisciplinary approach to bone health. Our team of physiotherapists and exercise physiologists work together to develop personalised programs based on your bone density, medical history, strength, mobility, and goals.
For those with osteopenia or osteoporosis, our ONERO® classes provide a safe, structured environment to build strength, improve posture, increase load tolerance, and support long-term bone health.
Equipment-based Pilates can also be integrated into your program to improve core stability, alignment, and movement quality – all essential for protecting the spine and preventing falls.
Whether you are navigating menopause, recovering from injury, or simply wanting to future-proof your bones, we can help you move with confidence.
When Should You Seek Support?
You may benefit from an assessment if you:
- are approaching or experiencing menopause
- have a family history of osteoporosis
- have been diagnosed with osteopenia or osteoporosis
- have experienced a previous fracture
- feel unsteady or concerned about falling<
- want guidance on safe, effective exercise for bone strength
A physiotherapist or exercise physiologist can help interpret bone density results (DEXA scans), identify risk factors, and design a program tailored to your needs.
Key Message
Your bones are continually adapting to the way you live, move, and care for your body. While ageing and hormonal changes are unavoidable, the choices you make today can have a profound impact on your long-term bone health. With the right support, exercise, and lifestyle foundations, you can stay strong, mobile, and resilient throughout life.
If you would like to improve your bone health or find out whether ONERO® classes are right for you, our team at The Body Refinery is here to support you.
_ _ _
References
- Cosman, F., et al. (2014). Clinician’s Guide to Prevention and Treatment of Osteoporosis. Osteoporosis International.
- Giangregorio, L. M., et al. (2014). Too Fit to Fracture: Exercise Recommendations for Individuals With Osteoporosis. Osteoporosis International.
- Zhao, R., et al. (2017). Resistance Training and Bone Mineral Density in Postmenopausal Women. Sports Medicine.
- Sherrington, C., et al. (2019). Exercise to Prevent Falls in Older Adults: Systematic Review and Meta-Analysis. British Journal of Sports Medicine.
- Watts, N. B., et al. (2022). Osteoporosis in Postmenopausal Women: Diagnosis and Monitoring. Journal of Clinical Endocrinology & Metabolism.